Evolution of mechanical ventilation
The use of mechanical tools to assist ventilation dates back to the late 19th century, when devices able to apply an alternating subatmospheric pressure around the body were used to restore ventilation by expanding the chest wall of patients [2]. However, it was only after the introduction of positive-pressure ventilation during the reappearance of poliomyelitis in the 1950s, when Bjorn Ibsen demonstrated a dramatic reduction of mortality in patients manually ventilated by tracheostomy, that mechanical ventilation started to be widespread [3].
The first positive-pressure mechanical ventilators became available in 1940. Though characterised by a significant degree of sophistication, they were able to deliver only a pre-set tidal volume at a given respiratory rate (volume-control ventilation mode) with no or very limited capability to monitor ventilation variables (figure 1a).

Figure 1
Evolution of the concept of mechanical ventilation. a) The first mechanical ventilators were not equipped with sensors. b) Mechanical ventilators monitor all the ventilation parameters, allowing both closed-loop control of the generated waveform and providing information to the clinicians. c) Mechanical ventilators monitor the condition of the patients and automatically adjust the ventilatory parameters on the basis of patients’ needs.
At that time, respiratory physiology had already established its foundations and was rapidly growing. The application of mathematical modelling to describe the relationships between flow and pressure (a wonderful example of what today would be considered a biomedical engineering approach), which marked the dawn of the mechanics of breathing, was introduced by Dixon and Brodie [4] in 1903, who modelled the lung as resistance and compliance. Rohrer [5] introduced a relevant simplification by considering only one pressure across the lung and one across the chest wall in 1915 (modelling confirmed by Mead et al. [6] in 1970), improving our capability to describe and understanding the mechanics of the respiratory system during both physiological and artificial breaths. Rahn et al. [7] introduced pressure–volume diagrams of the lung and thorax, and the concept of relaxation curves, in 1946, creating the background for the development of respiratory energetics. These and other studies constituted the physiological background that lead to the introduction of positive-pressure ventilation into clinical practice.
The main objective of mechanical ventilation was originally focused on restoring patients’ ventilation. This concept expanded as the other variables determining gas exchange were understood. Ashbaugh et al. [8] first described acute respiratory distress syndrome (ARDS) in 1967 and identified the positive end-expiratory pressure (PEEP) as “most helpful in combating atelectasis and hypoxæmia”. During the same period, animal studies showing oxygen toxicity when a high inspiratory oxygen fraction (FIO2) was used suggested increasing ventilation instead of FIO2 to treat hypoxaemia, leading to the (ab)use of increased tidal volume (VT).
From the early 1970s, ventilators benefited from the progresses in electronics, and started incorporating more advanced monitoring of flow and pressure variables (figure 1b). Improvements in monitoring also allowed the possibility of using real-time variables to control the action of the machine, with the intermittent mandatory ventilation mode opening the development of assisted mechanical ventilation as a way to manage the weaning of patients from periods of volume-controlled ventilation [9].
In the meantime, our understanding of the mechanics of breathing further improved thanks to the introduction of the concept of dynamic compression in airways during forced expiration by Fry, Hyatt and co-workers [10]; three-dimensional analysis of pressure, flow and volume curves [10, 11]; and a better understanding of chest wall mechanics from Campbell’s diagram for the partitioning of elastic and resistive work [12], and the two-compartment model of the chest wall by Konno and Mead [13].
In 1974, Webb and Tierney [14] demonstrated in animal models that ventilation with high distending pressures was leading per se to severe or even fatal pulmonary oedema, marking the beginning of a decades-long research effort aimed at understanding the adverse effects of mechanical ventilation and the mechanisms involved, and identifying appropriate strategies for preventing ventilation-induced lung injury (VILI), which despite the huge progress made so far, is still an open issue. Since then, major attention has been given to identifying the optimal ventilation strategy as a compromise between normalisation of blood gases and avoiding the development of VILI, resulting in the introduction of improved technologies for monitoring ventilation and lung conditions and the introduction of new advanced ventilation modes.
This progress was also possible thanks to the introduction of microprocessors in mechanical ventilators, starting in the early 1980s. Microprocessors are silicon electronic circuits able to execute programs; therefore, they can provide very complex functions that can be easily changed by selecting different programs, allowing a modern mechanical ventilator to rapidly modify its behaviour (e.g. changing from a volume-control to a pressure-control or a pressure-assist ventilation mode simply by selecting different control algorithms executed by the device). In addition, microprocessors allow the implementation of sophisticated signal processing of the measurements provided by sensors, leading not only to better measurement accuracy and better rejection of noise and artefacts, but also to the generation of new information by appropriately computing and integrating several variables. Moreover, this expanded information can be used by the ventilator itself to optimise the ventilation parameters on the basis of patient needs, creating the so-called “closed-loop” ventilation strategies or intelligent or smart ventilation modes (figure 1c).
The mechanical ventilator: the challenge of delivering accurate ventilation
Once a ventilation strategy is defined, the ventilator should deliver it to the patient in the most accurate way. To achieve this, the machine must sense all variables that define the breathing pattern with high accuracy and adjust its action in real time. Modern ventilators achieve this by combining cutting-edge technology of actuators, sensors and digital electronics together with sophisticated data processing algorithms. The basic components of a typical mechanical ventilator are shown in figure 2.
Summary:
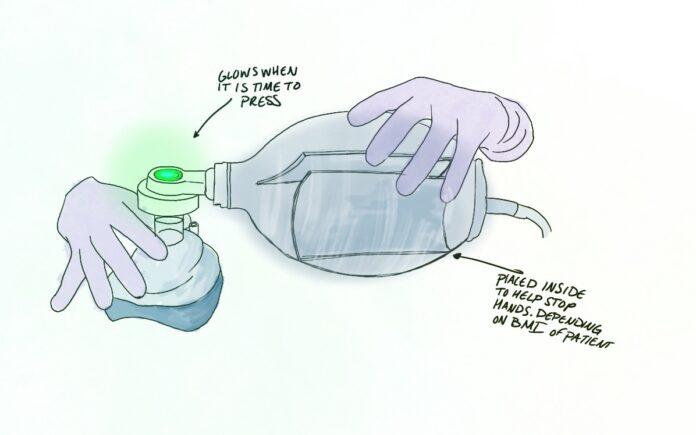
The current issue with manual ventilation is that people are all different shapes and sizes. This means different hand sizes, different strength in pressure, different pace. If pressure is too hard or fast than patients are more likely to die. The only way currently to deliver slow, adjusted breaths is for a machine to do it. A solution to manual ventilation could be that each breath is timed and a light goes off when the the bag no longer needs to be pressed and on when it is time to press the bag again. Another solution may be to create a stopper inside of the bag so that when your fingers touch the stopper you know you have pressed hard enough. These types of settings can be adjusted based on height, weight, and gender.